SWALLOWING DIFFICULTIES:
EOSINOPHILIC OESOPHAGITIS?
SWALLOWING DIFFICULTIES:
EOSINOPHILIC OESOPHAGITIS?
SWALLOWING
DIFFICULTIES:
EOSINOPHILIC
OESOPHAGITIS?
How is EoE diagnosed?
The diagnosis of eosinophilic oesophagitis (EoE) can only be made by a specialist (a gastroenterologist) after completing various investigations. The specialist will take a detailed history, analyse your symptoms and then carry out an endoscopic examination of the oesophagus. A number of small tissue samples (biopsies) will be taken of the lining of the oesophagus (the mucosa) during the procedure and then examined under a microscope by another specialist (a pathologist). With EoE, the biopsy of the oesophagus will normally show adverse changes in the cells of the mucosa which are consistent with inflammation and associated tissue damage. However, the diagnosis of EoE is only confirmed if large numbers of eosinophils (the specialised white blood cells) are present in the mucosa of the oesophagus.
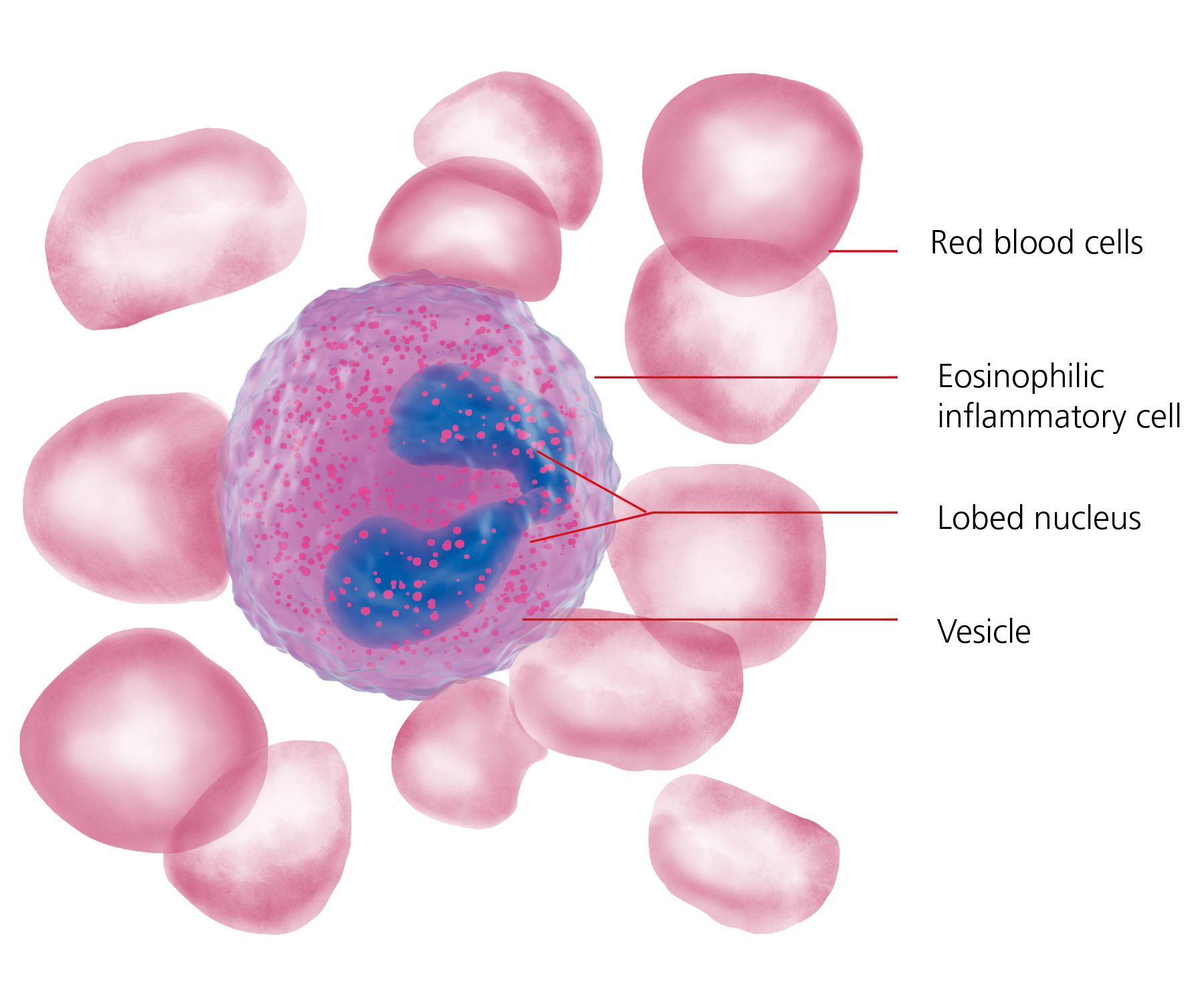

An eosinophil (a specialised white blood cell) surrounded by red blood cells. Inside the cell is a lobed nucleus (a compartment where genetic material is stored) and numerous vesicles (or granules) containing various substances which can cause inflammation and adverse changes in the oesophagus.
Each eosinophil contains a lobed nucleus and many vesicles. These store the substances that cause inflammation and tissue damage when the eosinophils release them. Eosinophils normally circulate in everyone’s blood and they play an important role in defending the body against parasites such as worms, and also are involved in the allergic response. Importantly, eosinophils are not normally found in the lining of the oesophagus (the mucosa) of the oesophagus, so their presence in large numbers in a biopsy of the oesophagus would be immediately noted as very unusual by a pathologist and would likely lead to the probable diagnosis of EoE.
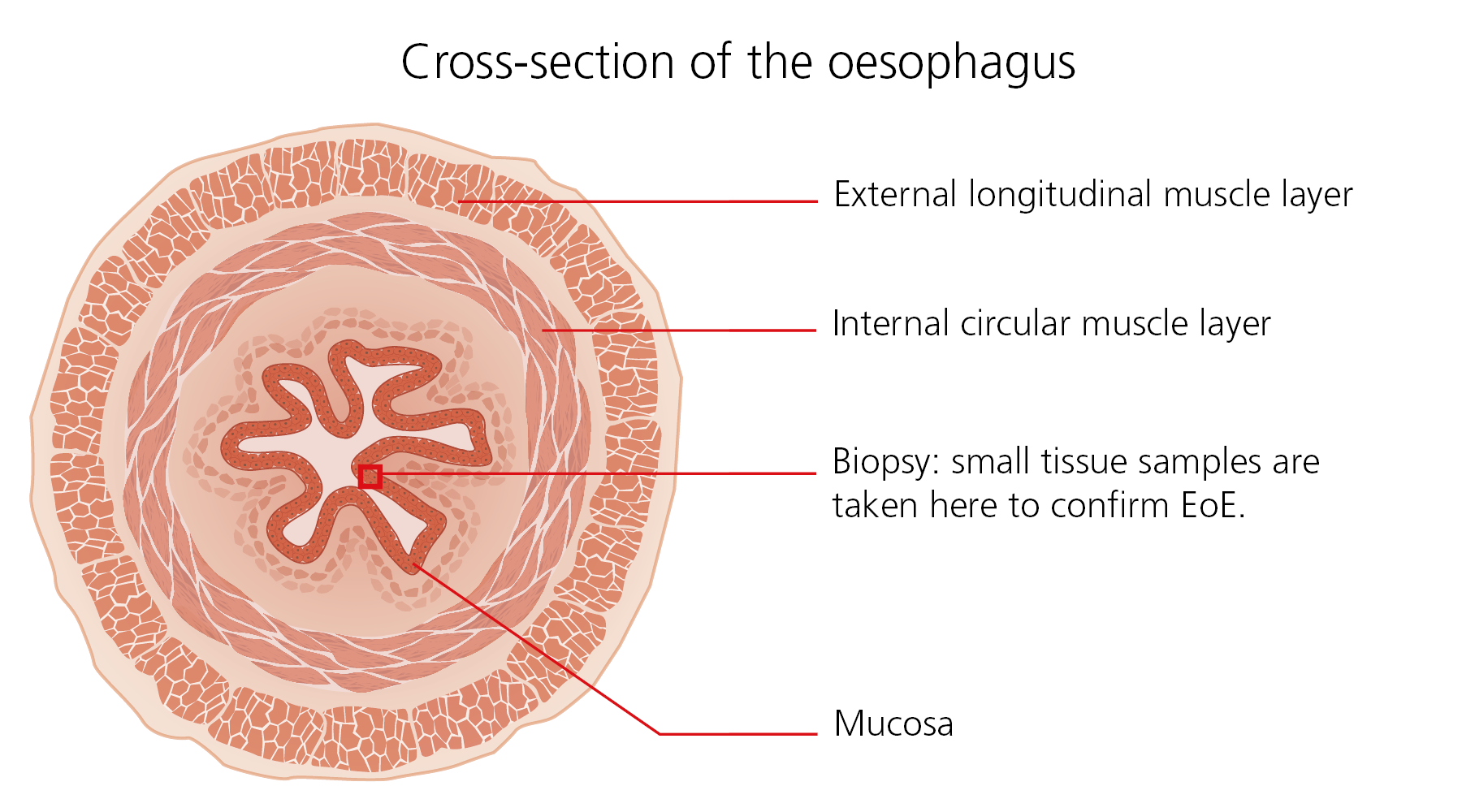

During a biopsy, several small tissue samples of the mucosa are collected in order to diagnose EoE.
Importantly, the biopsy allows specialists to exclude other conditions with some characteristics similar to those of EoE as part of the process to formally confirm the diagnosis.
